What is peritonitis?
Peritonitis is an infection of the peritoneum – this is a sheet of smooth tissue, called a membrane, that covers internal organs in the abdomen. Peritonitis is an infrequent but potentially serious complication of peritoneal dialysis (PD). It can have other causes (for example, as a complication of appendicitis), which is rare in people on PD.
Causes of peritonitis
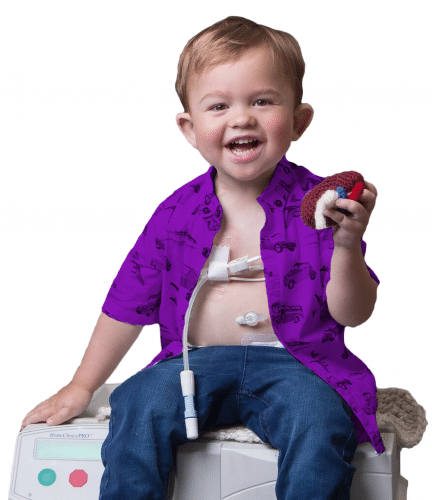
In continuous ambulatory peritoneal dialysis (CAPD) and automated peritoneal dialysis (APD), the peritoneum is used to filter out waste products and excess fluid from the blood.
Although rates are currently low and deaths are very rare, peritonitis can occur if bacteria enter the abdomen from outside the body through the tubing that allows this procedure to work (known as the dialysis catheter).
Peritonitis can occur if:
- Dialysis equipment is not kept clean (although in some cases, infection can happen even if every day is taken over hygiene).
- The open ends of the catheter are touched during a bag change which allows bacteria to enter the catheter.
- There is an infection around the exit site of the catheter.
- There is an infection of the large intestine (bowel) such as diverticulitis.
Peritonitis symptoms
The vast majority of PD peritonitis is very mild and easily treated with episodes typically less than one every two years.
Signs and symptoms of peritonitis can include:
- PD fluid that is cloudy or has visible white flecks – this is the most common and important sign and must be reported as soon as it is noticed.
- Abdominal pain – if experienced, always check if the fluid is cloudy
- Redness, pain or swelling at the catheter site – this should always be reported to the PD team
- Nausea and vomiting
- Rapid heartbeat
- Swollen abdomen
- High temperature
- Rigors: a medical term for episodes of severe shivering and a feeling of coldness
It is important that you contact your dialysis unit or the NHS 111 non-emergency medical helpline if you cannot get through to your unit and think you have peritonitis.
In severe cases, repeated bouts of infection can damage the peritoneum and cause thickening of the tissue (sclerosis) which can prevent peritoneal dialysis from working properly. Deaths are very rare and usually associated with underlying abdominal pathology.
Peritonitis diagnosis
If signs and symptoms are noticed, a small sample of PD fluid may be examined in a microbiology lab to look for the presence of white blood cells of which high numbers may indicate infection.
If white blood cell count is raised, PD fluid will also be ‘cultured’ (grown in a petri dish) to see which bacteria are causing infection and to determine which antibiotic treatments are suitable.
Two common types of bacteria are Staphylococcus epidermidis and Staphylococcus aureus (known as Staph infections), but many other bacteria can cause peritonitis, and occasionally infection can be caused by a fungus (usually Candida).
Peritonitis treatment
Peritonitis is usually treated easily with antibiotics. Antibiotic treatment is often started very quickly so that they can get to work whilst diagnostic tests are completed. If necessary, they may be adjusted to fit in line with any lab culture results.
Antibiotics can be added to new dialysis fluid, taken as tablets or more rarely, may be injected into a vein via a cannula. Some patients can administer treatment themselves at home whilst others may be treated at their local outpatient's department. In more severe cases, patients may need to stay in hospital for several days to receive more intensive treatment.
In rare cases, where individuals experience repeated bouts of peritonitis, haemodialysis may be required to rest the abdomen for several weeks or as a long-term treatment option. Sometimes, if part of the peritoneum has been seriously damaged by recurrent infection, surgery may be needed to remove it.
For some, peritonitis can cause difficulty in digesting food so a feeding tube might be passed into the stomach through the nose or placed in the stomach using keyhole surgery. If a feeding tube cannot be used, liquid nutrients can be given directly into a vein.
Prevention of peritonitis
Although infection is rare, it is important to prevent it by keeping dialysis equipment clean. This can include:
- Strictly following training given by the dialysis nurse particularly around exchange procedure and exit site care.
- Ensuring that the room for dialysis sessions is clean.
- Maintaining good personal hygiene before, during and after bag changes.
Resources and support of peritonitis
If you have any concerns about peritonitis or need help with your dialysis, do not hesitate to get in touch with your PD nurse or kidney specialist.
You can find helpful tips, advice and information about managing kidney disease on our website: How can I help myself? - Kidney Research UK
Further information about peritonitis can be found on the NHS website: Peritonitis - NHS (www.nhs.uk)
Reviewed December 2024
Our latest kidney research
Our research grants enable cutting edge research into all aspects of kidney disease

Could understanding blood pressure changes during sleep in kidney patients be key to protecting heart and vessel health?

New results suggest that bladder cancer could be caused by the body’s response to common childhood virus

SMC approval of mercaptamine offers new hope and choice for people living with cystinosis in Scotland

Research looking at repurposing drugs to treat polycystic kidney disease shows promising new results

Personalising treatments for focal and segmental glomerulosclerosis patients receiving a kidney transplant
Our life-saving research is only possible with your support.
Help transform treatments with your donation.